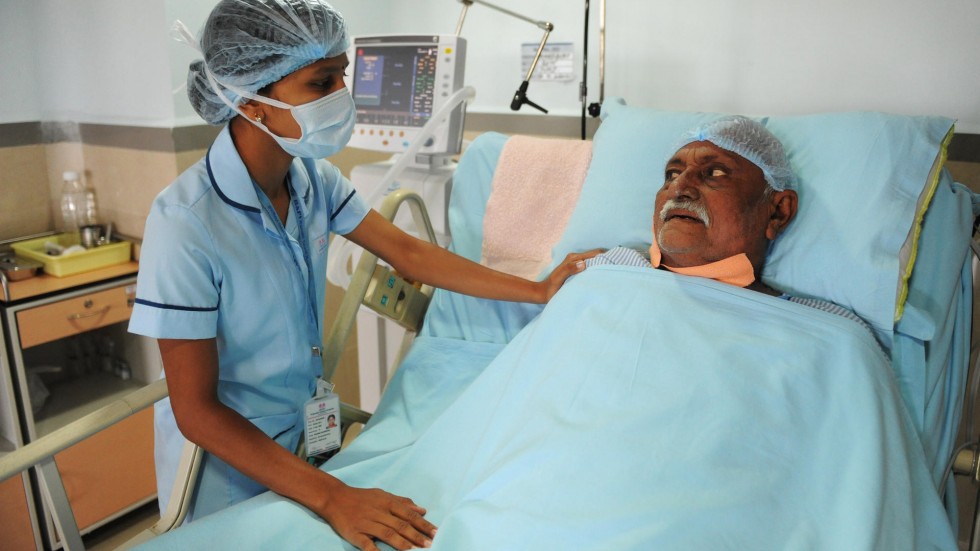
On India’s 72nd Independence Day, Prime Minister Narendra Modi announced the imminent launch of Ayushman Bharat or National Health Protection Mission (AB-NHPM), his government’s flagship project. The National Health Protection Scheme (NHPS) under AB-NHPM aims to cover 100 million vulnerable families (500 million individuals, 40 percent of the population) for up to $7,100 per year. The program, often labeled “Modicare,” is being described as the world’s largest health protection scheme.
This tag is easy to agree with: given India’s 1.3 billion population, any nation-wide scheme is likely to be one of the largest in the world. However, since only one in five Indians is covered by any form of insurance and out-of-pocket expenditure on treatment comprises 63 percent of the total health spending, an initiative that aims to bring down economic hardships of treatment on households merits careful consideration.
Stepping away from questions about the timing of the announcement (general elections are set to be held next year), the key question that needs an answer is whether the scheme is going to set India on the path of universal health coverage (UHC), meaning all Indians will have access to quality medical services and medicines without fear of financial hardships.
The NHPS by design leaves out ambulatory or outpatient care which means it excludes consultation, diagnosis, and treatment but includes hospitalization. It also leaves out expenditures on drugs outside of hospital settings – a major component of out-of-pocket expenditure1. Household data indicates that slightly more than half of all ailments reported get treated outside hospitals, in private clinics and lower tier health facilities.
Thus, the NHPS straightaway disqualifies to be a counted as a comprehensive scheme. However, the other initiative under AB-NHPM – Health and Wellness Centers (HWC) – aims to strengthen the lowest tier in the public health infrastructure. The HWCs will be the first contact points between patients and the primary health care system and are to address the basic care needs of the population. They can, in principle, form the missing half of the UHC: non-hospitalization care.
India’s Ailing Health Care
The timing of AB-NHPM’s launch, however, is of concern. Basic health care is badly ailing in India, especially in the rural areas, where there are huge shortages of facilities and medical personnel. The HWC initiative in its present form is unlikely to overcome these severe shortages in a time sufficient enough for it to keep up with the rollout of the NHPS. The target of setting up 150,000 HWCs is only to be met by the end of 20222, while the NHPS is slated to roll out this month. With severe infrastructural constraints in many states, it is hard to imagine the two initiatives coming together in time to actually act as a UHC precursor.
There are other, more pressing concerns about the NHPS, however, than just operational ones.
Current spending on health in India is about 4 percent of GDP of which the government spends about 1.1 percent. Governments with UHC spend a much higher share of their GDP on health care. While the shares of the U.K. and Canada are 7.9 and 7.7 percent, closer to India, China and Thailand spend 3.2 and 2.9 percent out of their GDP as government health spending. Over the years, public resources devoted to health have remained meager in India, raising issues of prioritization.
In addition to low government spending, high out-of-pocket expenditures, and inadequate public health infrastructure, India’s health sector is characterized by a largely unregulated and rapidly expanding private healthcare sector that is often charged with corruption and malpractice3. Low, fragmented, and iniquitous health coverage is another aspect.

The question is whether the NHPS will address these problems or will only add another layer of complexity to the already chaotic health sector. At the very least, is there evidence that similar hospitalization schemes have helped reduce out-of-pocket expenditures?
A decade ago, India launched the Rashtriya Swasthya Bima Yojana (RSBY), a government-funded scheme meant for the unorganized sector workers. The government did not evaluate RSBY, but evidence based on independent research4 indicates that the program has not helped the poor to reduce their out-of-pocket expenditure on hospitalization. To massively scale up an essentially similar model without first evaluating the reasons for the non-performance or impact of an earlier one does not seem like a good policy move. The RSBY has also been plagued with many administrative loopholes and concerns, and it is not clear if the new model will be able to address these issues. Clearly, given that the new NHPS is a much more expensive program, failure would be very costly.
Merging State Schemes with NHPS
While states are free to continue with their own health programs in addition to the NHPS, they can opt to merge their schemes with the NHPS. However, there is no evidence how and at what cost either of such systems would work, if they work at all. The administrative, managerial, and cost implications are serious enough to warrant detailed pre-launch research and planning. In any case, for states that are running “successful” schemes, there should be no compulsion to run the NHPS. The fact that a majority of states have agreed to do so could partly be due to the financial incentives that the NHPS throws up, and partly due to political contingencies.
Given the shortage of facilities in the government sector, the scheme plans to depend heavily on the private sector. The expectation that the NHPS would encourage private providers to set up facilities in areas where there are none is neither rational nor justified. With the current rates set by the government, it is unlikely that private providers would fill in the gap with offers of quality care; if the rates are revised, then the financial sustainability would be a critical issue. In any case, the prospect of further privatization of the health sector in an unregulated environment raises serious concern.

It is anyone’s guess what Modicare would actually cost since there is yet to be clarity on the specific models to be adopted by states, targeted coverage, and the situation with mergers with existing schemes. The health ministry initially allocated about $1.4 billion, but clearly, the NHPS would require a much larger resource envelope: the scheme aims to rely significantly on technology and would require solid administrative and managerial support.
There are indications from the government that allocations are not a problem, and funds would be available if required. However, that cannot happen unless the total resource amount for the health sector is enhanced significantly at central as well as state levels, so as not to squeeze out other important investments.
The central government’s budget estimate for 2018-19 for the Department of Health and Family Welfare’s increased by a mere 2.4 percent compared to 2017-18, which does not seem commensurate with the increase required to support a scheme on the scale of NHPS. Similarly, since states would require to shoulder 40 percent of the costs, they would need to increase their currently low health allocations substantially. Past trends indicate that the increase in state health budgets has been quite modest. In the face of a constrained health budget, financing the NHPS should not be at the cost of other health sector investments.
This brings us to the last question: given scarce resources, could resources have been allocated differently to implement reforms that ultimately would have moved the country towards accessible, affordable, and quality care?
Investing in basic care, filling personnel and infrastructure gaps, pushing urgently on regulation reforms, reforming medical education, revamping procurement of drugs and devices would possibly have required similar funds if done incrementally, but with more concrete, visible, and expected outcomes. Countries that have moved on the path of UHC have mostly undertaken similar reforms in a phased manner. However, these are now moot questions: the juggernaut has been launched; the costs of adopting the NHPS and of foregone opportunities comprise a separate issue that still needs to be answered.
1 Selvaraj S, Farooqui HH, Karan A. Quantifying the financial burden of households’ out-of-pocket payments on medicines in India: a repeated cross-sectional analysis of National Sample Survey data, 1994–2014. BMJ Open 2018;8;e0180202. doi:10.1136/bmjopen-2017-018020 2 Government of India, MOHFW, Rajya Sabha, Unstarred question no. 1553, answered on 31.07.2019: New health and wellness centers 3 Parliament of India. Rajya Sabha. Ninety second report. The Functioning of Medical Council of India (Ministry of Health and Family Welfare). March 2016 4 Karan A, Yip W, Mahal A. Extending health insurance to the poor in India: An impact evaluation of Rashtriya Swasthya Bima Yojana on out of pocket spending for healthcare. Social Science & Medicine (1982). 2017;181:83-92. doi:10.1016/j.socscimed.2017.03.053Disclaimer: The views and opinions expressed here are those of the author and do not necessarily reflect the editorial position of The Globe Post.